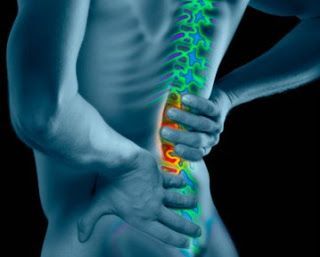
Low back pain can be felt anywhere below the ribs and above the legs.
The condition is very common that almost everyone has experienced it at one point in their lives or another.
Treatment options for low back pain can range from noninvasive alternatives to surgery.
However, it is recommended that checking with orthopaedic specialists would be ideal so the best treatment alternative will be provided.
Causes
While low back pain can be attributed to a lot of things, below are some of the most likely causes:
- Pressure placed on the nerve roots – this can be attributed to other medical conditions like a herniated disc or a spinal stenosis.
- Injury or overuse – this involves sprains and strains on the soft tissues like the ligaments and the muscles. The condition can also be traced to injuries in the small joints found between the bones of the spine or to compression fractures of the bones.
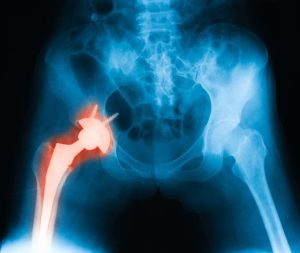
- Osteoarthritis – when the condition affects the small joints situated in the spine, it can become the cause of back pain. Osteoarthritis in other joints such as the hips can also change how an individual walks resulting to back pain.
Other conditions that can likely cause low back pain include:
- Bacterial infection
- Spinal tumors
- Ankylosing spondylitis
Symptoms
Depending on what causes it, low back pain can have diverse symptoms.
For instance:
Back sprain or strain
Usual symptoms can include:
- Cramping, muscle spasms, and stiffness
- Pain in the buttocks and back that may come and go
Nerve-root pressure
Usual symptoms can include:
- Numbness, tingling, and weakness in one leg or both
- Pain in the leg (in majority of the cases, the pain will start in the buttocks and will travel back to the foot, leg, or ankle)
- Loss of bowel or bladder control (this can also be a symptom for cauda equine syndrome and will need immediate medical attention)
Osteoarthritis
Osteoarthritis in the spine can result to pain that:
- More severe in the back and hip region
- Starts gradually but can become severe eventually and can last up to 3 to 6 months
- Gets worse after long periods without any activity
Treatment
Orthopaedic specialists diagnose, assess, and can recommend the best treatment alternatives for back pain.
Most cases of low back pain do not necessarily require a visit to an orthopaedic specialist.
However, if the pain gets too severe and it gets to a point where it hinders the patient from going about their usual routine, getting medical attention becomes a must.
Back pains are divided into two categories—acute and chronic.
Acute
Pain lasts less the 3 months but will respond to home remedies.
Chronic
Pain lasts more than 3 months and will require intensive treatment.
Treatment options for acute low back pain
If pain has persevered for a few days and does not respond to any noninvasive remedies (using heat or ice, taking painkillers, etc.), other treatment options like stronger pain medications and manual therapy might be recommended.
For those who experience severe pain, short-term use of opiate painkillers or muscle relaxants might be prescribed.
Epidural steroid shots might also be recommended.
Treatment options for chronic low back pain
For back pains that are chronic, one type of treatment will often not suffice.
Possible treatment options can include:
- Cognitive-behavioral therapy
- Massage
- Acupuncture
- Comprehensive rehabilitation programs
- Biofeedback
Since low back pain can have different causes, treatment approach can vary from one individual to another.
To play safe, it would be best to have the condition assessed by a seasoned orthopaedic specialist so the best treatment option can be identified.
Is low back pain keeping you sidetracked? Visit www.bjios.sg for help.